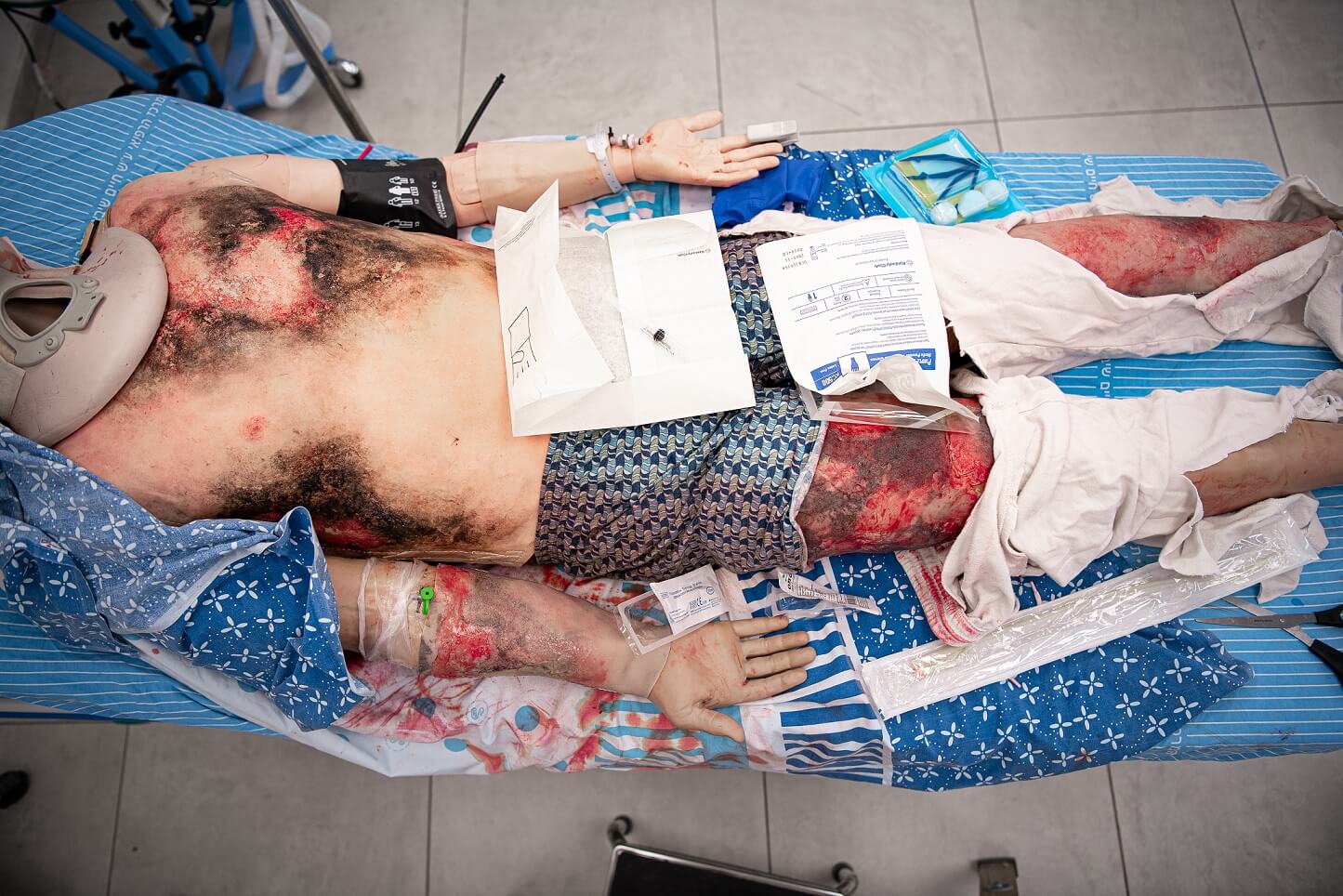
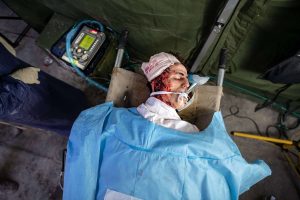
How do you offer a realistic training experience to the medical staff? What are the things you should take into account, and how do you offer feedback?
We reached out to a medical professional, Dr. Sarit Shahrur Hadar, who is a former head of the children’s intensive care unit in Shaare Tsedek hospital in Jerusalem. We wanted to learn firsthand what the expectations are from a medical expert on the proper way to go through medical training.
We also discussed important points to consider during epidemic outbreaks such as the current Covid-19 pandemic, and we also got her feedback on the right training tools and mannequins for the medical industry.
Below you can find a transcript of our conversation. Feel free to send us a message and let us know your thoughts on this interview.

How do you train your medical staff for emergency scenarios, assuring the best outcome in a future emergency event?
Sarit: “Traditional methods of educating residents and medical staff using lectures and bedside teaching are no longer sufficient. The expanded medical knowledge, the highly technical environment and the complexity of clinical situations necessitate using a different, hands-on approach.
We have found that simulation-based resuscitation training, for example, is an excellent active-learning tool.”
How is the realistic, hands-on training method different from your past training experience? Do you feel that hyper realistic medical training solutions are contributing to improving the skills of medical teams?
Sarit: “In these simulations, the medical team copes with realistic situations created within a physical space which replicates a real-life environment.
Simulation-based training provides a learning opportunity for controlled clinical practice without putting patients at risk.
Simulations of clinical scenarios help the medical staff to prepare for actual events, practice the required interventions in a safe environment, identify team weaknesses and improve their technical skills and teamwork.
These benefits are less available through the old traditional learning process.”
What are the challenges of training physicians in emergency care?
Sarit: “In order to get an optimal outcome of resuscitation, simulation training is essentially needed. This training was adopted as the standard in medical professions. It is characterized by complex, dynamic environments in which crises evolve rapidly and the risk to human life is high.
Mannequin simulators provide some of the most realistic and high-yield environments for trainees and are accepted as valuable training tools.”

Considering outbreaks like the Covid-19, what is the best way to prepare for an epidemic like this in the future?
Sarit: “In March 2020, the WHO (World Health Organization) declared the COVID-19 outbreak a pandemic. It urged all countries to take action in detecting infection and preventing spread.
Here in Israel, I am a member of the Sprint Corona team. Its goal was to optimize the coping measures and treatment options of Covid-19 patients.
At that time there was limited knowledge about the disease, the epidemiology, its management, as well as the best treatment to offer patients. It was obvious that we had to move fast and gather professional teams to deal with limited resources and lack of knowledge.
Almost six months later, we know that the outcome of Covid-19 patients depends on the “saturation level” of medical teams, their ability to be trained fast in critical mass casualties, and the appropriate medical supply in each country.
The countries which implemented early and extensive measures, coordinated responses and pooled resources did well. Countries had to bring down the “reproducibility number” of the virus so that the health system could cope with the virus’ continued spread.
Fast training, which enables medical teams to deal with increased numbers of patients, is possible, especially by using simulations-based training.”
What should be learned from providing care in pandemics such as Covid-19? What are, in your opinion, the essential resources that help medical staff to cope with pandemics like this?
Sarit: Since March 2020 everything in the medical industry has changed, and future outbreaks (such as COVID-19 or other viruses) can occur anywhere.
Lessons are emerging about what is required to withstand the next outbreaks. Countries should be alert, share information, cooperate and set international regulations to ensure source control.
COVID-19 has challenged the medical societies: physicians must be open-minded, question their treatment options, share their knowledge and experience fast, and change treatment guidelines as the pandemic spreads.
While medical knowledge and experience are being accumulated from all over the world, hospitals must train medical personnel to take care of medical emergencies and critical care scenarios.
This is where the simulation-based training method rules. The simulation of clinical scenarios is the best way to share medical knowledge fast. It allows you to train within a short time frame and with reduced resources while ensuring an increased learning curve, the recognition of a team’s weaknesses and potential obstacles.
This would fold into the best outcome and results dealing with a pandemic such as COVID-19.”
What would the ideal trauma mannequin look like?
Sarit: “The first mannequin simulator was developed by Abrahamson and Denson in the early 1960s and was initially used for anesthesia training. Since then, we have used mannequins to simulate extreme clinical scenarios almost weekly. Medical teams have been training in critical care units to learn how to cope and respond to similar extreme situations.
The best simulation of a medical emergency or clinical situation should imitate the real world in as much detail as possible. This includes sounds, sight, and smells, crowded environments, as well as common obstacles that teach the medical staff to handle similar real-life situations. Simulation can be used to demonstrate physical findings that would not be possible by other means.
High-fidelity mannequin simulation appears to have the highest promise in the training of physicians and may affect patient outcomes in real life.
High-fidelity simulation is rapidly becoming accepted as an advanced teaching tool for medical providers in all stages of practice. The high-fidelity mannequin simulator (HFMS) is a dynamic, computer-controlled, full-sized, simulated mannequin capable of giving a history, recreating physical exam findings (such as normal and abnormal heart sounds, lung sounds, and pupil findings), as well as physiologic changes (including blood pressure, heart rate, and breathing).
Some HFMS are even capable of physiologically responding to medication and oxygen administration, receiving electrical cardioversion, and procedures such as diagnostic peritoneal lavage and central lines.
This is the best way to train your medical team and achieve the best outcome. HFMS can be used to ensure that all physicians training in the care for the acutely ill (such as trauma or emergency patients) would acquire the necessary knowledge and skills to achieve the best results when dealing with these situations in real life.
Challenge us: do you have a specific requirement for extreme medical training?
The Extreme Simulations staff is ready to offer you high-fidelity medical training experiences that prepare you and your team for extreme situations. If you want to prepare your team for medical emergencies, contact us now
GET IN TOUCH
Contact Extreme Simulations now to book a complete training session